 Eczema is a form of dermatitis, or inflammation of the upper layers of the skin. Eczema is an allergic, inflammatory and irritating skin condition which causes dryness and recurring rashes on the skin. Some of the common symptoms of eczema are redness, skin edema, itching and dryness, crusting, flaking, blistering, cracking, oozing, or bleeding. Based on these symptoms, eczema can divided into three main types - acute, subacute and chronic Eczema is a form of dermatitis, or inflammation of the upper layers of the skin. Eczema is an allergic, inflammatory and irritating skin condition which causes dryness and recurring rashes on the skin. Some of the common symptoms of eczema are redness, skin edema, itching and dryness, crusting, flaking, blistering, cracking, oozing, or bleeding. Based on these symptoms, eczema can divided into three main types - acute, subacute and chronic
If you suffer from eczema, looking after your skin is vital to control the condition and reduce the number of flare-ups you experience.
General skin care, applying moisturisers and avoiding factors that trigger your eczema are the most important things you can do.
After that, treatment of eczema often involves several different approaches to control the condition and all its symptoms, and medicines of several different types may be used in combination.
Dry Skin:
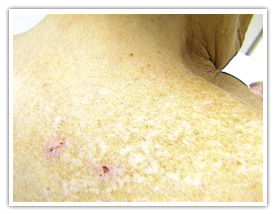 Aside from avoiding trigger factors, the most important element of eczema treatment is to keep the skin hydrated by regularly using moisturisers and moisturising soap substitutes. Aside from avoiding trigger factors, the most important element of eczema treatment is to keep the skin hydrated by regularly using moisturisers and moisturising soap substitutes.
These help to maintain the barrier function of the skin and reduce itching, scratching and the penetration of irritants, allergens and micro-organisms.
Moisturisers should be used regularly, even when using other treatments and when the condition seems to have cleared up.
They have been shown to reduce the number of flare-ups of eczema, which are experienced, and therefore reduce the need for topical corticosteroids.
Inflammation:
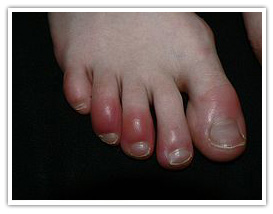 Flare-ups of eczema are traditionally treated with topical corticosteroids. These reduce inflammation in the skin and are safe and effective medicines when used correctly. Flare-ups of eczema are traditionally treated with topical corticosteroids. These reduce inflammation in the skin and are safe and effective medicines when used correctly.
Topical steroids come in various strengths, and the least potent product that is effective should be used to control the inflammation.
Mild corticosteroids are generally used for children and on the face and flexures, eg crease of the elbow or behind the knees etc.
More potent corticosteroids may be needed for adults with discoid or lichenified eczema, or with eczema on the scalp, limbs, and trunk.
Once the inflammation is under control, topical steroids should be reduced to the mildest strength needed to control the eczema, or if possible, stopped. People using topical steroids should be regularly reviewed by their doctor.
There are two steroid-sparing treatments for reducing inflammation and controlling flare-ups, called tacrolimus and pimecrolimus.
They are calcineurin inhibitors and work in a different way to steroids to suppress the inflammatory reactions in the skin.
They're not associated with the same potential side-effects of steroids and are an important advance in the treatment options for eczema. However, they are usually reserved for when corticosteroids have not been effective or cause unacceptable side-effects. Sometimes, they can cause an initial burning sensationon the skin.
It's advised that they should be applied intermittently, to active areas of eczema only, and patients should limit sun exposure, in order to reduce any potential skin cancer risk.
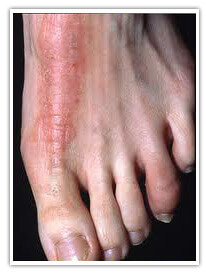 Lichenification: Lichenification:
Lichenification is thickening of the skin with exaggeration of the normal skin markings, which gives the skin a leathery, bark-like appearance.
It's a result of repeated scratching and is initially treated with potent topical corticosteroids.
Bandages are sometimes applied over the topical steroids to treat chronic, lichenified eczema, because these increase the absorption of steroid into the thickened skin and break the ‘itch-scratch’ cycle of eczema. They should only be used under the supervision of a doctor.
The bandages may sometimes contain zinc, ichthammol or coal tar, used for their anti-itching and mild anti-inflammatory effects.
Infection
Chronic eczema may often become infected, particularly with the bacteria Staphyllococcus aureus, which is found in large numbers on skin affected by eczema.
Eczema in moist areas of skin such as skin folds is also more susceptible to fungal infections. Infection worsens the inflammation of the skin and may require treatment with antimicrobial medicines, such as antibiotics, antifungals or antivirals.
Depending on the severity of the infection, antimicrobials may be either applied to the skin or taken by mouth. If the eczema is frequently infected a doctor may prescribe moisturisers and moisturising bath additives that also contain antiseptics to try and prevent infection.
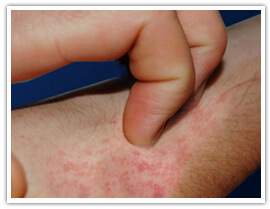 Itching Itching
Many people complain that itching is the worse symptom of their eczema.
Scratching makes itching worse because it increases inflammation and increases the likelihood of the skin becoming infected.
So, short courses of sedating antihistamines are sometimes prescribed to help reduce severe itching during acute flare-ups of eczema.
These are mainly of value because they cause sedation, and are usually taken at bedtime to help sufferers sleep without scratching.
Unresponsive or Very Severe Eczema
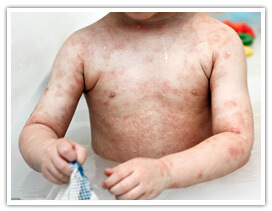 Occasionally, eczema may respond poorly or not at all to all the treatments mentioned above, and in these cases the patient will be referred to a hospital specialist. However, there is cure for eczema. There are various treatments that can subsequently be tried for very severe eczema. Occasionally, eczema may respond poorly or not at all to all the treatments mentioned above, and in these cases the patient will be referred to a hospital specialist. However, there is cure for eczema. There are various treatments that can subsequently be tried for very severe eczema.
A course of corticosteroids taken by mouth may finally bring the inflammation under control. Alternatively, immunosuppressant medicines, such as ciclosporin or methotrexate, may be tried to modify the skin’s inflammatory responses.
These are powerful medicines that require a good deal of monitoring to minimise the risk of side-effects. But adults and children with severe eczema, who do not respond to other treatment, can benefit greatly.
Light treatment (phototherapy) is another option for unresponsive and severe eczema.
People with eczema often comment that sunshine improves their skin, and light treatment is sometimes offered in hospital dermatological centres.
UVB light therapy for eczema can be extremely beneficial – as can PUVA which involves a combination of a drug called psoralen taken by mouth, followed two hours later by UVA light treatment.
Short-term side-effects of light treatment include sunburn-like reactions, and potential long-term side-effects include premature skin ageing and skin cancer.
Alitretinoin capsules are another option for chronic hand eczema, a form of eczema that's notoriously difficult to treat. However, it's a new treatment and not widely used yet.
Natural / Ayurvedic Treatment for Eczema:
Natural Treatment and Ayurvedic Cure for Eczema
The doctors of Ayusya herbal clinic have given the patients wonderful recovery from those all forms of eczematous skin providing best medicines derived from highly effecacious herbs from medicinal point of view and guided patients to perform following measures for achiving best and fast recovery.
 Boiling the bark of the babul tree in water and fomenting the affected areas with its fumes gives relief Boiling the bark of the babul tree in water and fomenting the affected areas with its fumes gives relief- The seeds of the butea are mixed with lime water and are applied on the affected regions to get the required benefits.
- Carrot juice and spinach juice in combination is highly beneficial for eczema.
- Add 1 teaspoon to 1 teaspoon camphor sandalwood paste and apply on the affected areas.
- For moist or weeping eczema, apply, in neat or cream form, Red clover or Hearteas.
- Tomato juice is regarded as an effective medicine which clears up the eczema in a matter of days.
- Applying the juice of the wild almond (Terminalia catapa) on the affected parts provides relief.
- Both drinking and applying externally over the affected parts, a brew of the peel of banyan tree shows promising results.
|

 Aside from avoiding trigger factors, the most important element of eczema treatment is to keep the skin hydrated by regularly using moisturisers and moisturising soap substitutes.
Aside from avoiding trigger factors, the most important element of eczema treatment is to keep the skin hydrated by regularly using moisturisers and moisturising soap substitutes. Lichenification:
Lichenification:
 (0)9831775590
Book appointment
(0)9831775590
Book appointment
 (0)9831775590
Book appointment
(0)9831775590
Book appointment
 (0)9831775590
Book appointment
(0)9831775590
Book appointment
 (0)9831775590
(0)9831775590
 (0)9831775590
(0)9831775590
 (0)9831775590
(0)9831775590



 Eczema is a form of dermatitis, or inflammation of the upper layers of the skin. Eczema is an allergic, inflammatory and irritating skin condition which causes dryness and recurring rashes on the skin. Some of the common symptoms of eczema are redness, skin edema, itching and dryness, crusting, flaking, blistering, cracking, oozing, or bleeding. Based on these symptoms, eczema can divided into three main types - acute, subacute and chronic
Eczema is a form of dermatitis, or inflammation of the upper layers of the skin. Eczema is an allergic, inflammatory and irritating skin condition which causes dryness and recurring rashes on the skin. Some of the common symptoms of eczema are redness, skin edema, itching and dryness, crusting, flaking, blistering, cracking, oozing, or bleeding. Based on these symptoms, eczema can divided into three main types - acute, subacute and chronic Flare-ups of eczema are traditionally treated with topical corticosteroids. These reduce inflammation in the skin and are safe and effective medicines when used correctly.
Flare-ups of eczema are traditionally treated with topical corticosteroids. These reduce inflammation in the skin and are safe and effective medicines when used correctly. Itching
Itching Occasionally, eczema may respond poorly or not at all to all the treatments mentioned above, and in these cases the patient will be referred to a hospital specialist. However, there is cure for eczema. There are various treatments that can subsequently be tried for very severe eczema.
Occasionally, eczema may respond poorly or not at all to all the treatments mentioned above, and in these cases the patient will be referred to a hospital specialist. However, there is cure for eczema. There are various treatments that can subsequently be tried for very severe eczema. Boiling the bark of the babul tree in water and fomenting the affected areas with its fumes gives relief
Boiling the bark of the babul tree in water and fomenting the affected areas with its fumes gives relief